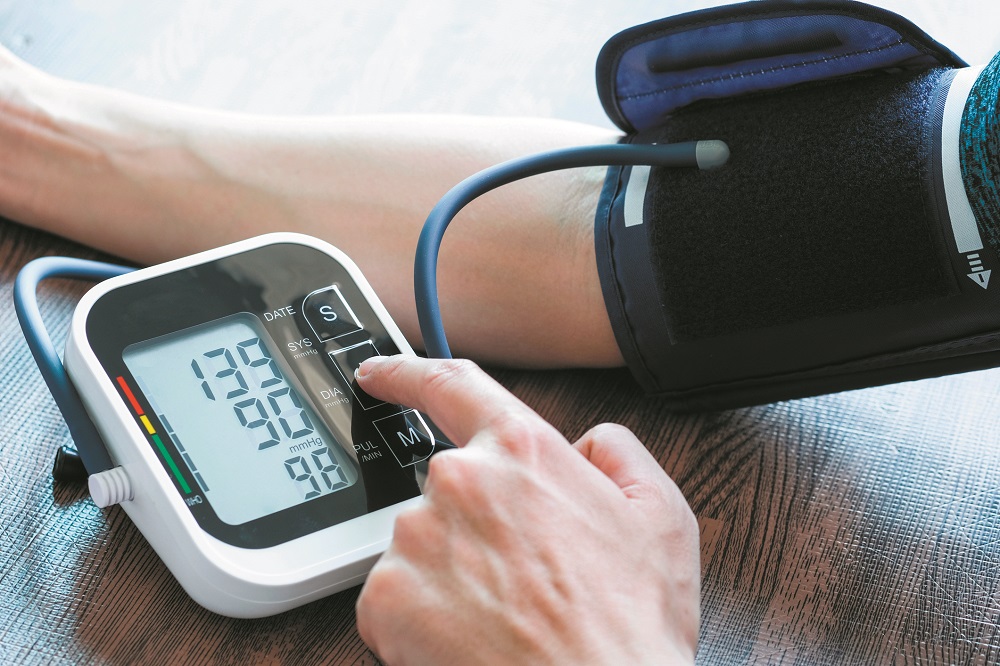
High blood pressure—we hear about it every day. Most of us know someone who has high blood pressure, or perhaps you have it yourself. That’s not surprising since about half of all US adults have high blood pressure, also known as hypertension.
What you may not know is how dangerous it is. High blood pressure is the single leading risk factor for mortality. In fact, it is the primary or a contributing cause of death for nearly 700,000 people in the US every year, according to CDC estimates. It is a leading contributor to stroke and a range of cardiovascular problems and kidney disease…and it’s a major risk factor for developing cognitive impairment. Scary stats, right?
But there is good news, says Mayo Clinic hypertension specialist Gary Schwartz, MD. High blood pressure is extremely preventable and treatable. Just making a few lifestyle changes could dramatically reduce your risk or help control an existing blood pressure problem. In fact, some hypertension self-care strategies are just as effective as medication. But even when drugs are needed, the ones that reduce blood pressure are effective, affordable and generally very well-tolerated.
The Silent Killer
When people type “hypertension” into a search engine, they often encounter lists of symptoms that include severe headaches, chest pain, dizziness, difficulty breathing, nausea/vomiting, blurred vision and more. You might conclude that if you don’t have these symptoms—and you don’t feel physical tension or pressure—you must not have high blood pressure. Don’t believe it!
High blood pressure typically is completely asymptomatic—the symptoms listed for the condition generally appear only after hypertension is extremely advanced to very high levels or has caused serious damage to the heart, brain or kidneys. Much of the harm from high blood pressure occurs before any symptoms appear.
Reality: There is only one reliable way for you to know if you have hypertension—have a health-care provider check. Smart watches and phone apps that monitor blood pressure may be useful—if one of these devices reports high blood pressure, it certainly is worth mentioning to your health-care provider. But these devices have not yet been extensively evaluated, so don’t depend on their readings alone.
New Blood Pressure Targets
Recent research has led to a reevaluation of what constitutes healthy blood pressure. Historically health-care providers were likely to recommend treatment when systolic blood pressure (the top number) was above 140 and/or diastolic blood pressure was above 90. But the Systolic Blood Pressure Intervention Trial (SPRINT), a large-scale study funded by the National Institutes of Health, persuasively showed that mortality levels are significantly reduced when the lower targets of 130/80 are used instead. Result: Hypertension treatment now is recommended for many patients who would not have been treated in the past…and the treatments they receive often are more aggressive.
Hypertension Self-Care
The best news is that we all have a substantial amount of control over our blood pressure. An Italian study concluded that genetics contribute only a relatively modest 30% of hypertension risk…the remaining 70% can be dramatically affected by lifestyle and diet decisions. Among the self-care options to consider if you are diagnosed with hypertension or wish to avoid that diagnosis…
Lose weight. Being overweight roughly doubles risk for hypertension…and if you have hypertension, losing weight will lower your blood pressure.
Reduce salt consumption. Multiple studies have identified a link between high salt consumption and high blood pressure. High-salt diets also can reduce the effectiveness of medications prescribed to lower blood pressure. Try to consume no more than 1,500 mg to 2,300 mg of sodium per day.
Increase potassium intake. A recent study by University of Modena and Reggio Emilia, Modena, Italy, in Journal of the American Heart Association found that consumption of 3,500 mg to 5,000 mg per day of potassium helps lower the blood pressure of people who have hypertension. For reference, one average-sized banana has around 450 mg of potassium…one avocado, around 500 mg.
Studies also support the notion that a low-sodium, high-potassium diet reduces risk of developing hypertension. In societies that naturally consume such diets, which are rich in fresh fruits and vegetables, hypertension affects a much smaller percentage of the population, whereas in societies like ours that consume a diet high in sodium and low in potassium, almost 50% of the population develops hypertension.
Helpful: The Dietary Approaches to Stop Hypertension diet (DASH diet, for short) was created by the American Heart Association to help people who have high blood pressure determine what to eat. It works—studies have found that following this low-sodium, fruit-and-vegetable–rich diet reduces blood pressure as much as any single medication, even without weight loss. Type “DASH diet” into a search engine for details.
Engage in aerobic activity. Many studies have found that aerobic exercise reduces blood pressure—try to get at least 150 minutes per week.
Limit alcohol intake. The evidence is strong that excessive alcohol consumption increases risk for hypertension—and that includes the consumption of red wine, which has sometimes been portrayed as good for heart health. Men who have high blood pressure shouldn’t consume more than two alcoholic drinks per day…women, no more than one per day.
Limit caffeine intake. Consuming large quantities of coffee or other highly caffeinated beverages appears to increase blood pressure…at least temporarily. The evidence here is less certain than it is with alcohol, but if you have hypertension, limit yourself to no more than one to two cups of coffee or other caffeinated beverages per day.
Try respiratory strength training. A study by researchers at University of Colorado found that using a “resistance breathing training device” (shown at right) for just 30 breaths a day for six weeks significantly lowers blood pressure. The inhaler-shaped device, which makes it harder to inhale, strengthens breathing muscles when used regularly. These devices are widely available for less than $100.

Keep stress under control. While there is no evidence that stress is a direct cause of hypertension, it can trigger many things that have been found to increase blood pressure, including sleeplessness, overeating and alcohol use. So using stress-control techniques such as mindfulness training or meditation could make it easier to keep your blood pressure under control.
When Medication Is Needed
Hypertension treatments are not difficult for patients—it is typically one pill once a day. The drug prescribed likely falls into one of three classes—diuretics…calcium channel blockers…or renin-angiotensin-aldosterone system (RAAS) inhibitors. Drugs in this class include angiotensin-converting enzyme inhibitors (ACEs) or angiotensin receptor blockers (ARBs). Their effectiveness varies from patient to patient for reasons that are still being researched. Affordable generic versions are available…and significant side effects are uncommon.
Patients should not be surprised if their health-care providers later prescribe additional medications—approximately 75% of high blood pressure patients respond better to a combination of drugs than to a single drug. But even then, it often is possible to take a single pill because drug companies make tablets that include common combinations of hypertension drugs. The combination pill usually consists of two of the drugs mentioned for single-drug treatment—for example, a diuretic plus a calcium channel blocker or ACE/ARB.
Some patients worry that taking high blood pressure medications could lead to orthostatic hypotension—where blood pressure drops suddenly when the patient stands up, causing dizziness and potentially falls. While orthostatic hypotension is a legitimate concern, health-care providers should test for this risk by taking the patient’s blood pressure while he/she is seated and immediately after standing. But this is not a reason to not treat hypertension. New finding: A recent study by a team of researchers at institutions including Harvard Medical School found that intensive blood pressure–lowering treatment actually seems to decrease risk for orthostatic hypotension.