Chronic sinusitis is a common condition that affects up to one in 20 people in the United States. Yet many people who have it never get properly diagnosed because they blame their symptoms on something else—usually allergies. Getting an accurate diagnosis and the right treatments could help a lot of people breathe easier.
Similar to asthma
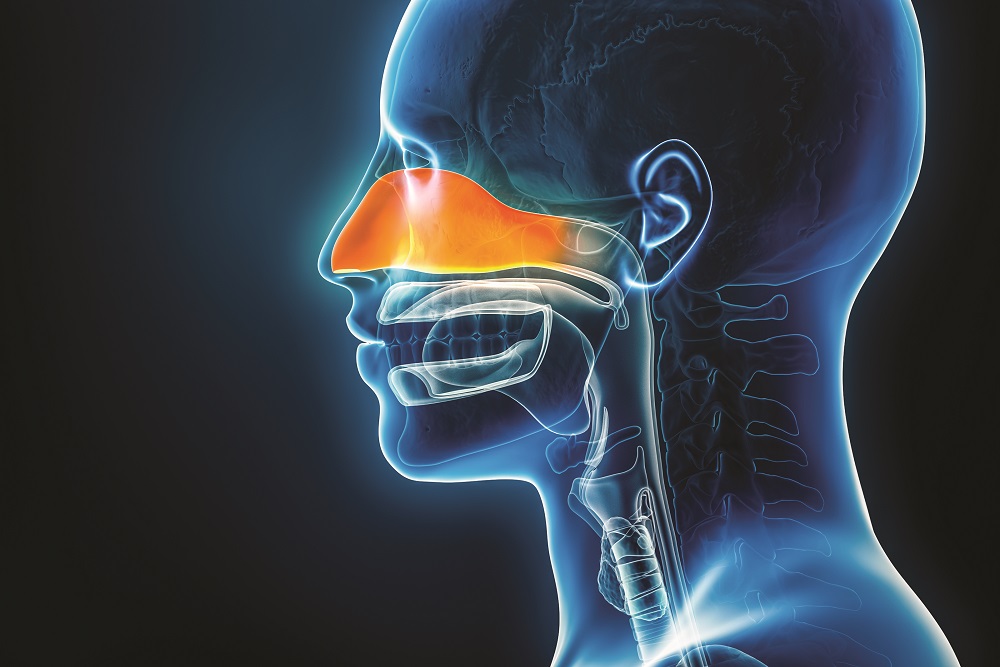
Chronic sinusitis (or, more accurately, rhinosinusitis) is an inflammation of the nasal passages and sinuses that lasts for at least three months. The typical symptoms include facial pain or pressure, a congested or dripping nose, and a diminished sense of smell. Many people with chronic sinusitis also have nasal allergies, which can make symptoms worse. But the allergies aren’t the underlying cause.
Unlike the acute attack of sinusitis you might get after a cold, chronic sinusitis isn’t usually caused by infection. While people with chronic sinusitis can get sinus infections, their symptoms persist even when the infections are gone.
In fact, chronic sinusitis is a condition much like asthma. People with asthma have inflamed airways in their lungs that swell and produce excess mucus in response to a variety of triggers. People with chronic sinusitis have tissues in their nose and sinuses that overreact in much the same ways. Pollen, viruses, bacteria, or fungi might trigger the inflammation, but so might cigarette smoke or other forms of air pollution. And what causes problems in one person may not in someone else.
Getting a diagnosis
If you feel like you have endless allergies or a cold that never quits, you might have chronic sinusitis. The big tip-off is having at least two of these symptoms for at least three months:
- Facial pain or pressure. Your sinuses are air-filled spaces in your forehead, cheeks, between your eyes, and deeper within your head. When the tissue lining those spaces swells and fills with mucus, pain and pressure can result, even if no infection is present.
- Nasal congestion. While congestion from a cold typically goes away in a few days and congestion from allergies often comes and goes with the seasons or other changes in your environment, this congestion persists.
- A nose that drips, either through your nostrils or down the back of your throat (post-nasal drip). In most cases, the mucus is not colored. If you do see green or yellow discharge, it’s more likely you have a bacterial infection.
- A weak sense of smell. This also happens to people with some respiratory infections, including COVID-19. Whatever the cause, a lingering loss of smell can be a big deal, making your food less enjoyable and creating safety issues, since you might not smell smoke, hazardous fumes, or spoiled food.
In addition to these primary symptoms, some people with chronic sinusitis may cough because of post-nasal drip and feel pressure in their ears. Many people report poor sleep and fatigue or “brain fog.”
What to expect from the doctor
If your doctor suspects chronic sinusitis, you will need a test to confirm or rule out the diagnosis. One possibility is a CT scan, which can produce images of the inside of your head. The pictures can show any swelling inside your sinuses and whether you have polyps, noncancerous growths that can develop in inflamed sinuses and nasal passages. Not everyone with chronic sinusitis has polyps.
If you see an ear, nose and throat doctor, you will likely get a different test: a nasal endoscopy. For this procedure, done in the doctor’s office, a lighted scope will be passed up your nose so the doctor can get a good look at the nasal lining. Unless you’ve had sinus surgery, the scope won’t fit through the narrow slits inside your nose that lead to your sinuses, but the doctor will be able to look for signs of inflammation, including thick mucus and any polyps in the area where the sinuses drain into the nose.
Also, the doctor will consider whether you might have other conditions linked with sinusitis. For example, some people with immune deficiencies are prone to sinusitis. So are people with forms of vasculitis, rarer conditions involving blood vessel inflammation.
Get relief
If you do have chronic sinusitis, there are two easy things you can try that make most people feel better:
- A nasal rinse, at least once a day. Rinsing the nasal passages with a saltwater solution (see sidebar) has been shown in multiple studies to help relieve symptoms. The rinses help to clear mucus and may also reduce inflammation by removing irritants, such as pollen and dust, from the nose.
- A corticosteroid nasal spray. You can choose any brand or generic version sold over the counter, such as fluticasone propionate (Flonase), triamcinolone (Nasacort), or budesonide (Rhinocort). These sprays, which also treat allergies, help lower inflammation and reduce congestion and runny nose. (To increase effectiveness, lean forward so that you are looking toward the floor; then aim the spray up and slightly to the side, away from the center of the nose, and sniff lightly).
An increasingly used alternative: With a doctor’s prescription, you can get a liquid corticosteroid that can be added to your saline rinse. This combo may help the steroid reach deeper into the affected sinuses.
Additional drugs might be used in some situations:
- Corticosteroid pills, such as prednisone. These might be used if you have polyps and severe symptoms. Because a steroid that affects your whole body can cause side effects such as sleeplessness and mood swings, they typically aren’t prescribed for more than three weeks at a time.
- Antibiotics. If you have a flare-up caused by a bacterial infection, you might get a short course of antibiotics. In some cases, doctors prescribe a certain type, called macrolide antibiotics, for a longer time, not to fight infection but to control inflammation.
- Biologics. Several newer injected drugs that target parts of the immune system involved in inflammation have been approved for people who have chronic sinusitis with polyps. While the drugs can be effective, they are extremely expensive. Right now, they are used sparingly.
If you don’t get relief from nasal rinses and medications, you might consider surgery. Using a scope inserted in your nose, a surgeon will remove any polyps and widen the openings of your sinuses to improve drainage and allow medications to better reach inflamed tissues. Surgery helps many people, but it’s not a cure, so you should expect to continue medications and nasal rinses after your procedure.
How to rinse your nose
Nasal rinses are an effective treatment for chronic sinusitis, if you do them correctly. A few guidelines:
- A little spritz from a tiny spray bottle is not enough. Use at least a cup of fluid in a large squeeze bottle, bulb syringe, or a neti pot.
- Most doctors recommend an isotonic saline solution, which has the same salt concentration as your body. A hypertonic solution, which is saltier, may be more effective, but also more irritating. Recipes (combining iodine-free salt and baking soda) are easy to find, but it’s worth buying premixed packets to make sure you get the right concentration. Add the mixes to distilled or boiled and cooled water.
- Whether you use a bottle, syringe, or a pot, bend over the sink (or in the shower) and gently squirt or pour the solution into one nostril at a time. Don’t worry about whether the fluid comes out the opposite nostril; that’s not possible for some people with blocked nasal passages.