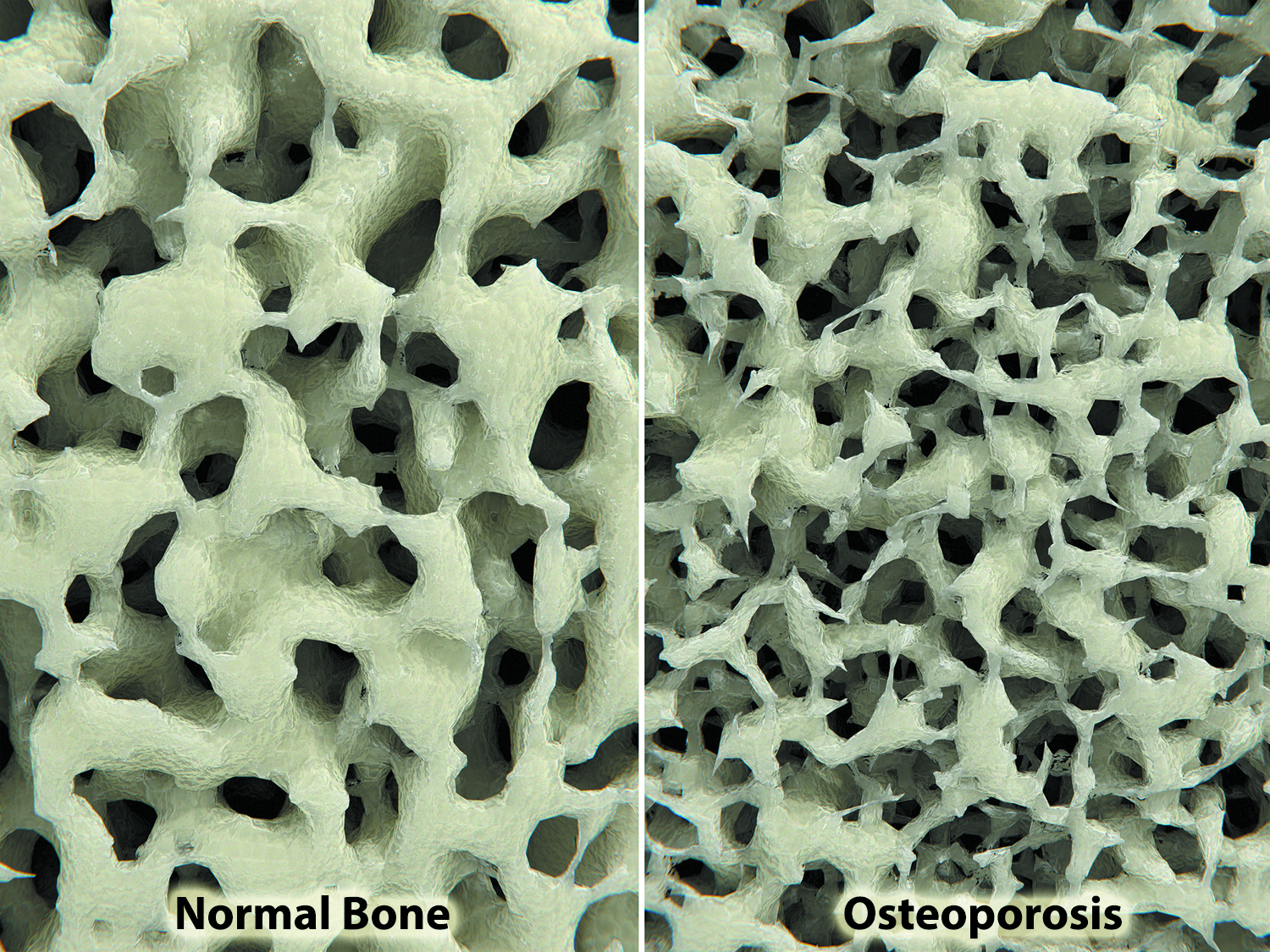
The results of your bone scan suggest you have a decline in your bone mass—something your doctor refers to as osteopenia. You’re familiar with the term osteoporosis, but what is osteopenia?
Osteopenia is a loss of bone density that, like osteoporosis, increases your risk for fractures. As bones become less dense, they become weaker and are more likely to break under stress or from a fall.
Lifestyle choices can slow bone density loss, but genetics and aging also play a big role in osteopenia. “Women are at greater risk of osteopenia than men because of rapid bone loss that can occur in menopause, and peak bone mass is higher in males,” says Cleveland rheumatologist Chad Deal, MD.
What is Osteopenia?
Clinicians use a bone density scan called dual-energy X-ray absorptiometry (DXA) to assess your bone health. A DXA scan is a special X-ray that compares your bone density to that of a population of healthy 25- to 35-year-old adults of similar sex and ethnicity. The DXA scan produces measurements known as T-scores, which suggest whether your bone density is lower than that population of adults.
Osteopenia is indicated when the score is between -1.0 and -2.5. If the score is -2.5 or lower, the diagnosis is osteoporosis, which is more advanced bone loss. DXA scans are generally recommended for screening in men over age 70 and women over age 65. Women between ages 50 and 65 may have DXA screening if they have risk factors for bone density loss, such as menopause, low body weight, height loss, a history of fractures or low vitamin D or calcium levels. Men younger than 70 may have a DXA screen due to a fracture or other risk factors.
Your physician may use a tool known as FRAX to assess your risk of suffering a major osteoporotic fracture (of the hip, spine, wrist, or humerus) in the next 10 years based on your DXA scan results and clinical risk factors such as age, sex, body mass index, smoking, drinking, family history, and corticosteroid use.
This tool helps determine when osteopenia treatment is needed. Since osteopenia is more common than osteoporosis and most people who suffer a fragility fracture have osteopenia and not osteoporosis, the use of FRAX is critical.
Osteopenia Medication
Based on your fracture risk, your physician may prescribe medications to help boost your bone density. They include oral bisphosphonates—e.g., alendronate (Fosamax), ibandronate (Boniva), and risedronate (Actonel)—as well as once-daily injections of abaloparatide (Tymlos), once-monthly injections of the dual-action anabolic medication romosozumab (Evenity), twice-yearly injections of denosumab (Prolia), and an intravenous infusion of zoledronic acid (Reclast), which is given every one or two years.
Bisphosphonates and other anti-resorptive medications prevent bone loss, whereas dual-action anabolic medications can help build bone while also preventing bone loss. Health-care providers recommend treatment when the FRAX score is high (greater than a 20% 10-year risk for major osteoporotic fracture, or at least a 3% risk for hip fracture).
Fight Osteopenia and Support Your Bone Health
Men generally lose bone density slowly over time, but they start with more bone than women. During menopause, women can lose bone density rapidly, and women often start with less bone mass than men.
“If you live into your 90s, most people have osteoporosis,” Dr. Deal says.
Genetics matter, as complex genetic factors we can’t control play a role in bone density loss. “Sometimes, I hear from someone who followed all the recommendations to prevent bone loss, yet they still have osteopenia or osteoporosis,” says Dr. Deal.
Bone loss is part of aging, but there are things you can do to help maintain your bone health, including a range of lifestyle practices. Adopting these bone-beneficial behaviors are critical for reducing your fracture risk, especially if you have osteopenia.
Take these steps to help prevent bone loss:
- Engage in bone-boosting weight-bearing exercise (e.g., walking, jogging, hiking, racquet sports) for at least 30 minutes a day on most days of the week.
- Get enough vitamin D, especially if you are vitamin D-deficient (have your vitamin D level checked at least once). Although the recommended dietary allowance is 600 to 800 international units (IUs) of vitamin D per day, many experts recommend getting at least 1,000 IUs daily. Good sources include fortified skim milk or orange juice, fatty fish (e.g., salmon, mackerel, tuna), and supplements.
- Get at least 1,000 to 1,200 milligrams of calcium a day. Good dietary sources include low-fat/fat-free milk and other dairy products, salmon, fortified cereals, and dark, leafy green vegetables.
- Stop smoking/using nicotine products. If you smoke, discuss cessation strategies with your health-care provider.
- Limit alcohol use to one drink per day for women or two drinks per day for men.