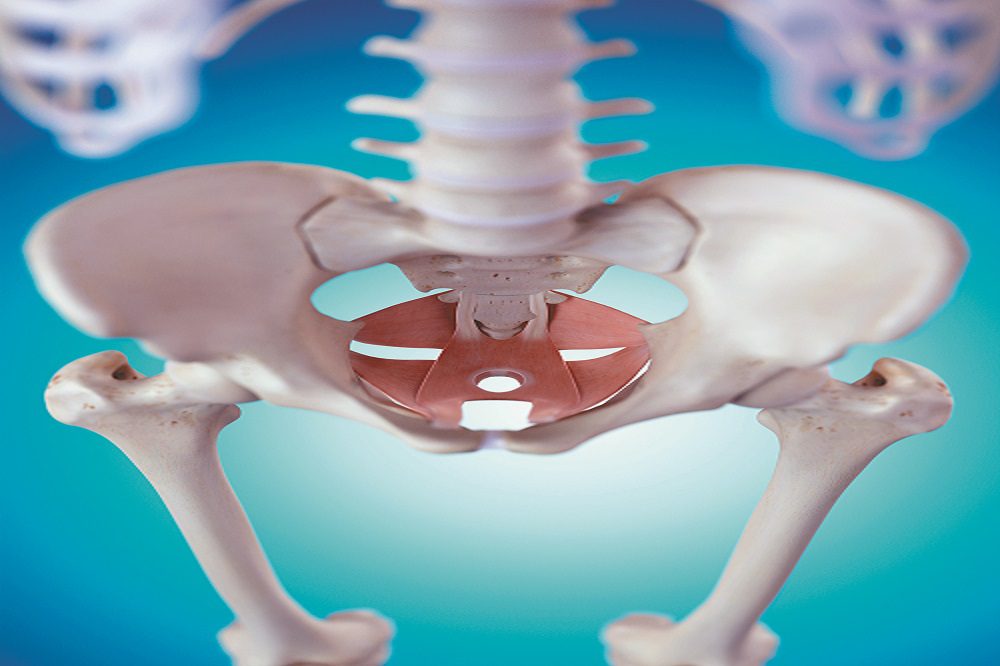
A well-functioning pelvic floor is important for both men and women for a number of reasons, all of which are easier to understand once you know where it sits within the body.
The pelvic floor is a sheet of muscles known as the levator ani with openings that allow canals, such as the urethra and the rectum, to pass through. There are sphincter muscles that squeeze these canals closed when you aren’t eliminating. The pelvic floor provides structural support to keep your organs, including the bowel and bladder—and the prostate for men and the vagina and uterus for women—in place when you jump, run, sneeze, cough and more. It is also essential for the stability of your spine and for good posture and is involved in sexual performance.
To identify exactly where your pelvic floor is: The next time you’re on the toilet—and your bladder is not overly full—deliberately stop the flow of urine just for a second (you will be using the same muscles used to prevent passing gas). Think of pulling up as opposed to pushing down.
Other ways to know if you’ve activating the right muscles: Sit on an arm of a couch. When you tighten the pelvic floor, you should feel your bottom lift up. Or sit on a cushion with a button and try to “pick up” the button with your butt.
When the pelvic floor doesn’t function optimally, you can experience incontinence, pelvic organ prolapse (when an organ, such as the uterus or the rectum, starts to come out of the body) and/or pain during sex for women and erectile dysfunction in men.
Common causes of a weak pelvic floor include…
Old age. As with other parts of the body, your pelvic floor simply may not work as well as it did when you were 30 years old.
Childbirth. Part of the levator ani can be torn during vaginal delivery and, unfortunately, the tear can’t be repaired, but healing, along with strengthening the other muscle sections, can help compensate.
Enlarged prostate or prostate surgery. Both can create challenges that the pelvic floor must deal with and lead to a weak urine stream or incontinence.
Strenuous exercise. Athletes—in particular, runners and weightlifters—who do intense exercise that puts significant demands on the pelvic floor may experience weakness and its negative effects. Example: Many female athletes on major university basketball teams leak urine when they play because the sport’s intense bouncing stresses the pelvic floor. While this isn’t damaging, it puts extreme demands on the system.
Obesity. Excess body fat presses down on the pelvic floor and can stress its muscle and ligaments. Studies show that losing as little as 15 pounds can reduce incontinence.
Reengaging Your Pelvic Floor
You can train your pelvic muscles to engage when you need them, easing urine leakage and other symptoms of a weak pelvic floor. You may have heard about Kegel exercises, but there are some misconceptions about how these help…how often to do them…and how to do them correctly.
What they are: Kegel exercises involve isolating the internal pelvic muscles and contracting them to activate and strengthen them. Contracting, or engaging, the pelvic floor is different from weight training a large muscle group. To understand the difference: You might strengthen your leg muscles to have the stamina needed to walk a golf course, but if you want to improve your putting, you aren’t heading to the weight room—you’re going to develop that skill so that, over time, it becomes a positive habit that takes over when needed. This is especially helpful if you have bladder leakage that’s bothersome but not to the point of requiring surgery.
There are many different approaches to pelvic floor training, but two are most successful…
The “Knack”: Janis Miller, PhD, a nurse practitioner and researcher at University of Michigan, suggests contracting the pelvic floor muscles in the moment, say when you’re about to cough or sneeze, to prevent leakage, rather than doing the exercises at set times during the day when you might not have any leakage risk. This technique is referred to as “the Knack maneuver”—you get into the habit of engaging that muscle at the precise time you need it. Once you get the knack of doing it purposefully and skillfully, your body may do it instinctively. Try it out before you need it: Pull your pelvic floor up and in, do a fake cough, and then relax your pelvic floor. Do this consistently whenever you feel an imminent leakage trigger coming on.
To determine if you are doing it right: Dr. Miller’s website, MyConfident
Bladder.org, offers a simple way to test if you’re contracting correctly and how well it’s working as well as many other practical ways to reduce or eliminate incontinence. The paper towel test is done with a modestly full bladder. Place three or four stacked paper towels against the urethra, cough three times without contracting the pelvic floor, and see how much wetness is on the towel, circling the wet area with a marker. Then repeat this using fresh paper towels and tightening the muscles as you cough, again circling any wetness with the marker. Compare the circles—if the wet area is reduced, you’re doing the Knack maneuver correctly.
More detailed training program: Another successful approach has been created by Kari Bø, PhD, exercise scientist and professor at Norwegian School of Sport Sciences in Norway. She has studied the pelvic floor extensively and works with patients who have an exercise lifestyle, are committed to keeping their body in shape and want to improve bladder weakness and/or sexual performance. You have to be highly motivated to improve your pelvic floor with her programs, but research has found that people who do her training for 20 minutes three times a week experience noticeable results.
For a 34-minute video on pelvic floor work: Go to https://bit.ly/2xrccnt.
For specific help with pelvic prolapse: Go to https://bit.ly/3Nm3N6r.
When Exercise Isn’t Enough
If contracting the pelvic floor on your own isn’t helping, work with a physical therapist who has special training in pelvic floor issues. Specialists who can help are urogynecologists, ob-gyns with three years of additional training, and, for men, urologists. You can look for one at VoicesForPFD.org/find-a-provider.