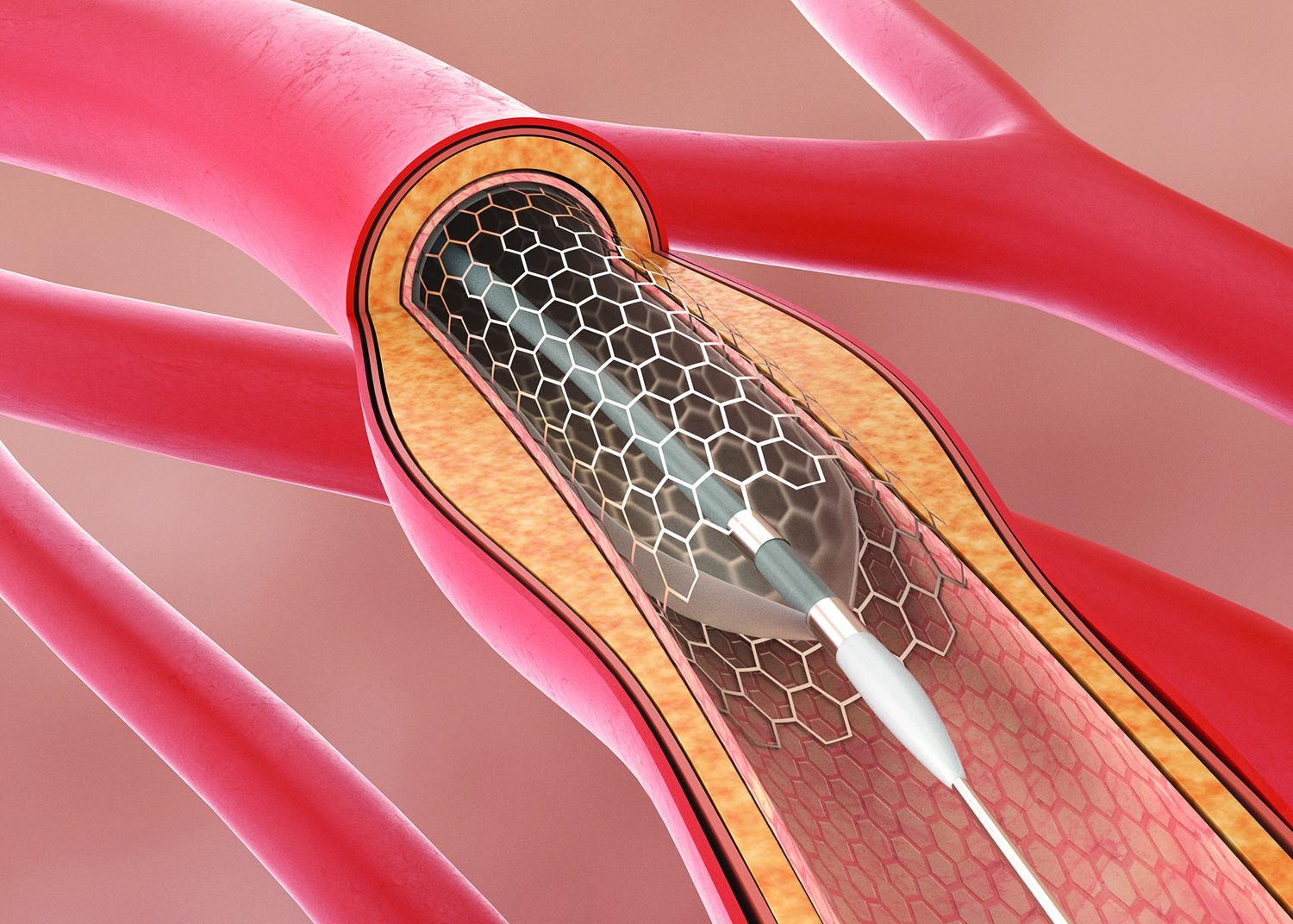
A heart stent is an expandable mesh tube that is placed inside a coronary artery to improve blood flow. Stents are used to push obstructing atherosclerotic plaque against the artery walls, clearing the way for better blood flow. Heart stents are not removed, but are left in the artery permanently to hold it open.
“Coronary artery stenting is used to achieve the same goal as coronary artery bypass grafting—that is, to prevent a heart attack and relieve the symptoms of coronary artery disease,” says interventional cardiologist Leslie Cho, MD.
Why You Need a Heart Stent
Your arteries and smaller blood vessels transport oxygen-rich blood to the cells, tissues and organs throughout the body. The coronary arteries, in particular, carry blood to the heart muscle, or myocardium.
Coronary artery disease occurs as a result of atherosclerosis, in which cholesterol and other fats and white blood cells accumulate and form plaques in the arterial walls. A narrowing or blockage in one or more coronary arteries caused by atherosclerosis restricts blood flow to the heart muscle and may eventually cause symptoms such as cardiac-related chest pain, known as angina.
Plaque buildup can fully block a coronary artery and cause a heart attack, or myocardial infarction. More commonly, heart attacks occur when a plaque ruptures and a blood clot forms in the artery, blocking blood flow and starving heart muscle of oxygen. The tissue in the part of the heart supplied by the affected artery begins to die. The degree of damage depends on the size of the area served by the blocked artery and how long it takes to restore blood flow to the affected heart muscle.
The Heart Stent Procedure
Heart stents are placed by interventional cardiologists or interventional radiologists in a percutaneous interventional procedure (PCI) known as angioplasty. Every year, about 445,000 of these procedures are performed in the United States.
A PCI is less invasive than surgery. “Percutaneous” means “punctured,” and the artery is accessed through a puncture made in the groin or wrist. A catheter tipped with a balloon and stent is inserted in the artery through the puncture site and advanced to the obstruction. The balloon is positioned inside the obstruction, inflated to push the stent against the artery wall, then deflated and withdrawn, leaving the heart stent behind permanently. Most patients go home the same day or the day after the heart stent procedure and have minimal discomfort.
Most heart stents in use today are made of metal and coated with a medication that slowly seeps into the artery to prevent the obstruction from recurring. Uncoated stents are known as bare-metal stents.
When Is a Heart Stent Used?
Angioplasty and stenting is the treatment of choice when blood flow must be quickly restored during a heart attack. In non-emergent situations, it is used in individuals who have one or two areas of obstruction and in those considered at high or prohibitive risk for surgery. Coronary artery bypass grafting (heart bypass surgery) is preferred over stenting in individuals with diabetes, a heart that pumps weakly and those with diffuse disease—that is, plaque throughout the arteries.
Another Type of Heart Stent
A stent in the heart also may be used in individuals with an aneurysm in their aorta, the largest blood vessel in the body. An aneurysm is a weakening of a blood vessel wall that results in an abnormal bulge or ballooning of the arterial wall. The force of blood against the aorta walls causes an aneurysm to grow larger.
In people with aortic aneurysms, a large stent made of metal and fabric may be inserted to create a barrier between the aorta wall and blood flow, effectively preventing the aneurysm from rupturing.