Each year, about 3% of older Americans are diagnosed with aortic valve stenosis. The condition forces your heart to work harder than it should, but because this extra exertion initially is asymptomatic, you may not be aware that your heart is beginning to struggle when it comes to pumping oxygen-rich blood to your body.
If aortic stenosis symptoms become noticeable, you may be able to alleviate them with lifestyle modifications and medications. However, Mount Sinai cardiologist Bruce Darrow, MD, PhD, notes that some research suggests that waiting for aortic stenosis to worsen before treating it surgically may not be the best approach for older adults who are otherwise fit and healthy.
“In these individuals, surgery has a good success rate and a low risk of complications, so it can make more sense to intervene before the condition worsens,” he says.
What Is Aortic Stenosis?
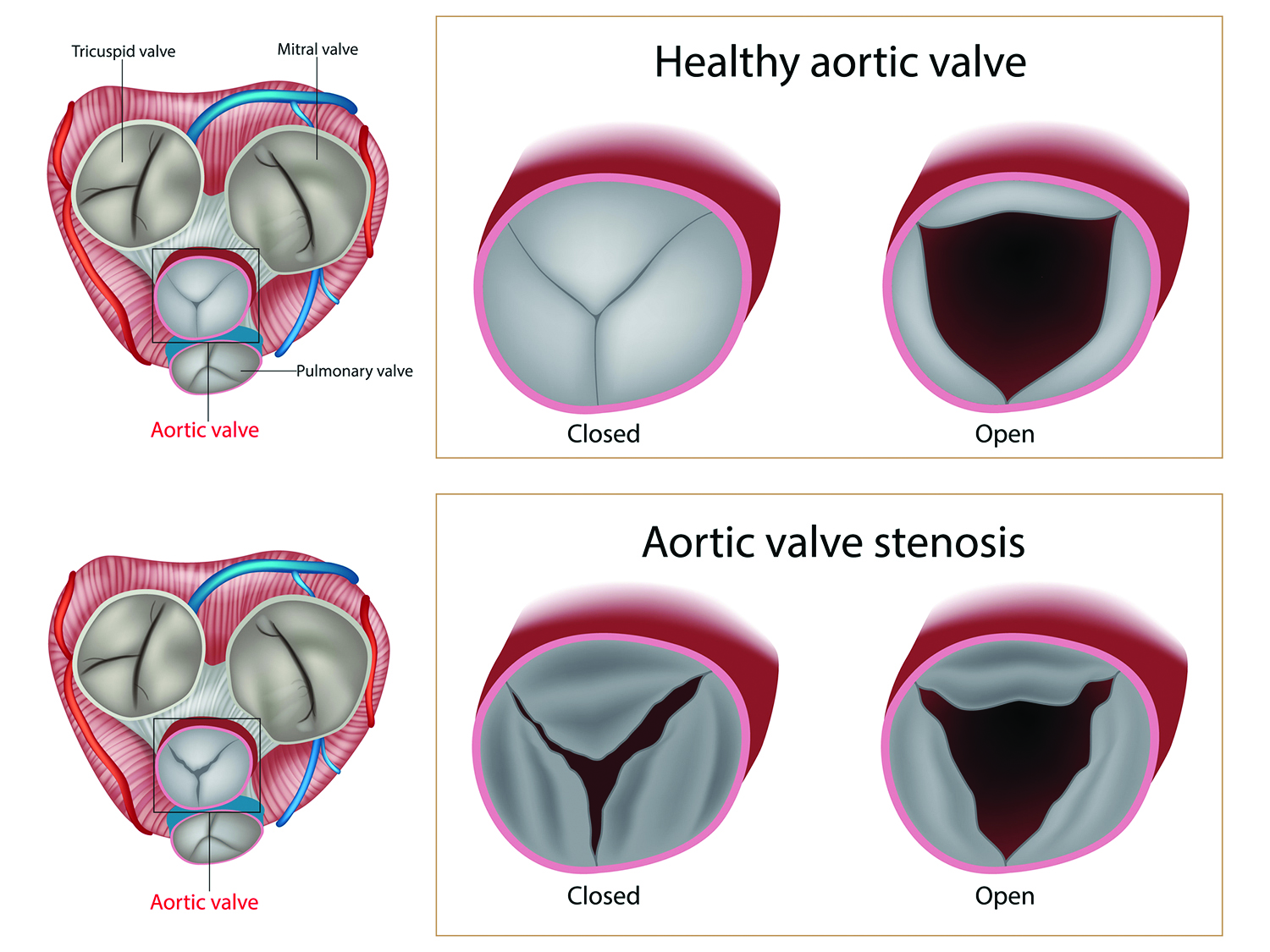
Your heart has four chambers, through which blood travels on its journey to your lungs and then back out to your body. Each chamber has a valve that opens and closes as needed to maintain forward blood flow through the heart. Stenosis—which can affect any of the four heart valves—narrows the valve. When this narrowing affects the aortic valve, your left ventricle (one of the two larger chambers at the bottom of your heart) has to work harder to pump blood into the aorta, the main artery leading from your heart to your body.
Just like any other muscle, your heart will thicken and enlarge in response to extra exertion. “This remodeling process helps your left ventricle pump blood out of your heart with more force,” Dr. Darrow explains. “However, working harder weakens your heart over time, reducing blood flow to your major organs.”
As your heart weakens, you may feel more fatigued than usual. Other aortic stenosis symptoms include feeling faint during physical activity, heart palpitations (which you may experience as a racing heartbeat or a fluttering/skipping sensation in your chest), and angina (a painful squeezing sensation in the heart muscle). If untreated, aortic valve stenosis can lead to heart failure, heart attack, and sudden cardiac death.
Aortic Valve Stenosis Causes
Aortic stenosis frequently is caused by a buildup of calcium in the valve. “Calcium is present in the blood, and as it flows through the aortic valve it can deposit on the valve’s three cusps,” says Dr. Darrow. “Cusps are flaps of tissue that form the valve. To function correctly, they need to remain thin and flexible, but calcium deposition stiffens them.”
This calcification process is common in older age but may affect younger adults if their aortic valve has only two cusps (known as a bicuspid aortic valve) or they have undergone radiation treatment to their chest (to treat cancer, for example). Calcification also may be increased in smokers, people with diabetes or chronic kidney disease, and those with high cholesterol and triglyceride levels.
Another possible cause of aortic valve stenosis is rheumatic fever, which can cause scarring of the heart valves. “Rheumatic fever is now rare in the United States, but elderly adults who had the condition in childhood may go on to develop aortic valve stenosis because the scarring can increase calcium deposition in the valve,” Dr. Darrow says.
Heart Murmur May Be a Clue
Many people are asymptomatic when diagnosed with aortic valve stenosis—the condition typically is detected during a routine annual physical if your doctor hears a heart murmur when listening to your heart.
“A heart murmur is a whooshing sound that may be caused by blood passing through a faulty heart valve,” Dr. Darrow explains. “If your doctor suspects a heart valve issue, you will be referred for imaging tests to confirm the diagnosis and evaluate how serious the problem is.”
Healthy Lifestyle Helps in Some Cases
Aortic valve stenosis usually isn’t caused by an unhealthy lifestyle, but if you aren’t experiencing aortic stenosis symptoms, lifestyle strategies will help protect your heart health. With this in mind, aim to consume a diet rich in fruits, vegetables, whole grains, low-fat dairy, and healthy fats, and get plenty of exercise to help you maintain a normal weight and improve cardiovascular risk factors like high blood pressure.
Drugs Can Mitigate Heart Damage
Medications that may be beneficial for people diagnosed with aortic valve stenosis include angiotensin-converting enzyme (ACE) inhibitors, beta-blockers, and diuretics. “ACE inhibitors can help slow ventricular enlargement, beta-blockers help to lower your heart rate, and diuretics help reduce the heart’s workload by decreasing the amount of fluid in your body,” Dr. Darrow says.
A 2025 Mayo Clinic study suggested that an investigational drug called ataciguat may slow the progression of valve calcification. In the study, the researchers detected a nearly 70% reduction in aortic valve calcification progression with ataciguat, compared with a placebo, at six months. People who took the drug also had better cardiac function and had fewer increases in left ventricular mass, compared with those receiving the placebo.
“There is an unmet need for pharmaceuticals that slow aortic valve calcification,” says Dr. Darrow. “These are preliminary data, but the results are promising. If the benefits seen are borne out in larger studies, people with aortic stenosis may have an effective pharmaceutical option that could delay surgical intervention or even make it unnecessary.”
When to Consider Surgery for Aortic Valve Stenosis
Up until recently, surgery to replace a failing aortic valve typically was recommended only when stenosis began to cause severe symptoms. However, some studies have suggested that managing the condition through “watchful waiting” may not be the best approach, given that even asymptomatic aortic stenosis irreversibly damages the heart and advances in surgical techniques have made valve replacement a relatively low-risk procedure.
“If you are asymptomatic, it’s important to factor in your health status if you are thinking about surgical intervention,” Dr. Darrow advises. “Many studies enroll people with few co-existing conditions and a low risk for complications. While surgery may be feasible for these individuals, it may not be the best choice for frail elderly people with asymptomatic stenosis.”
Valve replacement surgery involves transplanting a mechanical or biological valve in place of the failing valve. Each type of valve has pros and cons. “For example, mechanical valves are more durable and last longer, so they may better suit people who are younger when they undergo surgery,” Dr. Darrow says. “However, they raise the risk of blood clots, so people who receive them need to take anticoagulant medications for the rest of their life.”
Biological valves are made from animal tissue or other nonmetallic materials or may be taken from a donated heart. “A biological replacement valve is less likely to cause a blood clot, but it won’t last as long as a mechanical valve,” Dr. Darrow notes. “For that reason, older people are more likely to receive a biological valve.”
Surgical Procedures for Aortic Valve Stenosis
Most valve replacement surgeries carried out in the United States use a minimally invasive approach called transcatheter aortic valve replacement (TAVR), which can be performed under sedation. “During TAVR, a balloon catheter with a collapsible replacement valve at the tip is inserted into the femoral artery through a small incision and guided into the heart,” Dr. Darrow explains. “The catheter positions the replacement valve within the existing valve, and the balloon is expanded to open the replacement valve. The balloon is then deflated and the catheter is withdrawn.”
Recovery after TAVR typically is faster and easier compared with surgical aortic valve replacement (SAVR), and it offers a solution to older adults who may be deemed too frail for open surgery. However, Dr. Darrow cautions that some research has associated TAVR with a risk of postoperative stroke and arterial damage at the catheter insertion site. “There also isn’t yet much data on the longevity of valves replaced using TAVR,” he adds.
SAVR requires a 6- to 8-inch incision down the center of the sternum (breastbone), which then must be separated to allow the surgeon to access the heart. During the procedure, your heart will be stopped temporarily, and you’ll be placed on a heart-lung bypass machine that will oxygenate your blood and pump it to your organs. After the old heart valve is removed, a new valve is stitched into place and checked for leaks. If all is well, you’ll be taken off the bypass machine and once your heart is beating normally again and blood is flowing as it should, your sternum will be repaired and your incision closed.
“Valves replaced using SAVR may last for up to two decades,” Dr. Darrow says. “But the surgery is considered high risk for people whose left ventricle is failing, and for those who have had a previous heart attack. The recovery time also is typically longer than with TAVR—several weeks compared with just a few days.”
Get Informed
If you are considering aortic valve replacement, it is vital to have an in-depth discussion with your doctor about what surgical method is safest and most effective for you. “Just as importantly, keep in mind that beyond the surgical method used, your recovery and continuing well-being depend on following healthy lifestyle approaches that protect your heart health as well as mitigate other conditions you may have,” Dr. Darrow says.