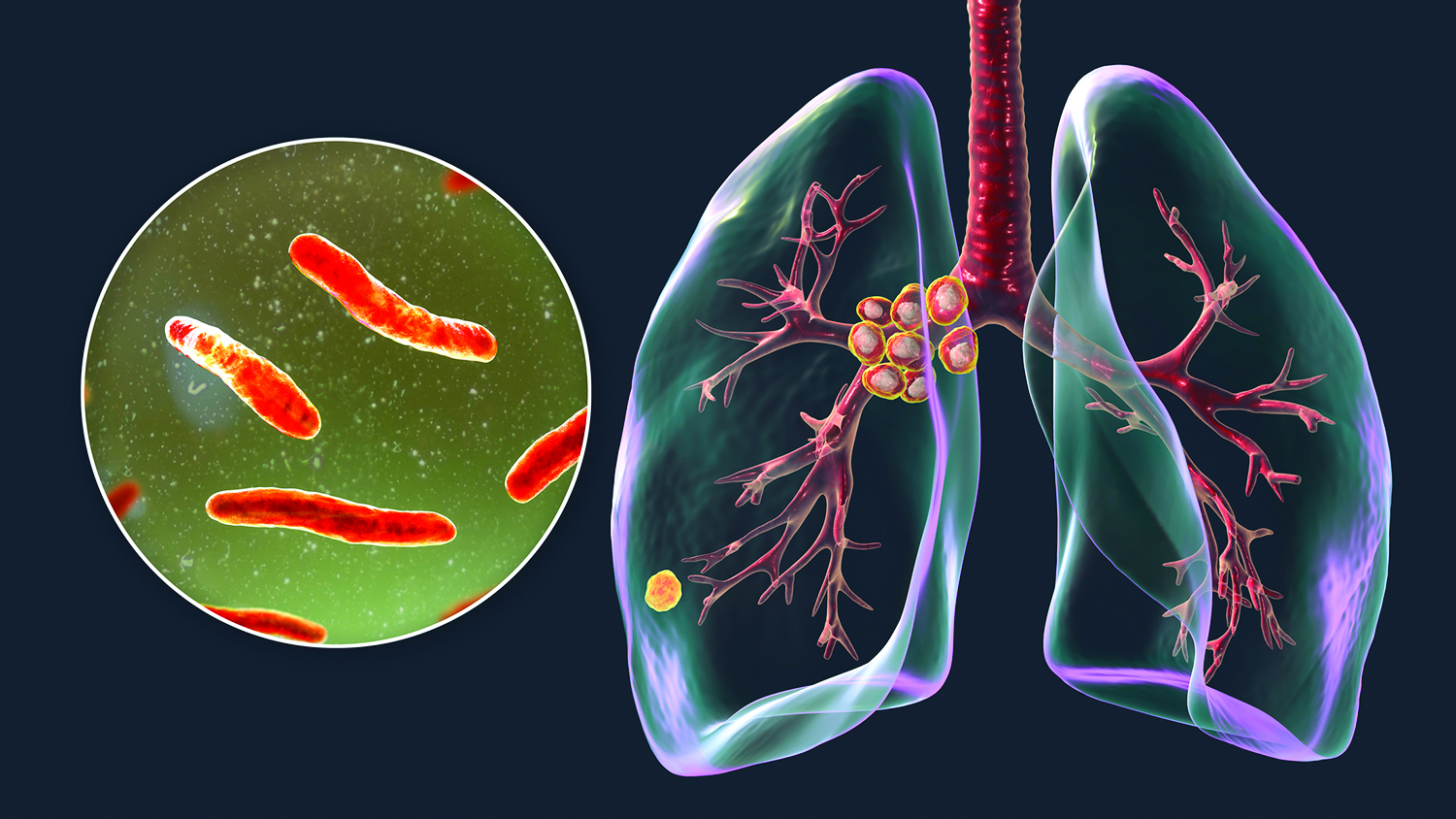
Tuberculosis (TB) is one of the oldest infections known to humankind. It primarily affects the lungs, although it can also affect other parts of the body.
Over the last several years, experts have noted an increase in cases worldwide. In 2024, the Centers for Disease Control and Prevention reported 10,347 cases in the United States—an 8% increase over 2023 and the highest number of new cases since 2011.
“Older adults are at particular risk for TB due to age-related weakening of the immune system that increases their risk for new TB infection from the community, and because of infection due to reactivation of old/latent TB,” says Sarah Taimur, MD, an infectious disease specialist at Mount Sinai.
She adds that the bacterium that causes TB—Mycobacterium tuberculosis (M. tuberculosis)—can be spread from person to person in the case of active TB. This transmission is especially likely when the infection is severe, since more serious illness means that a larger number of bacteria is present in the lungs.
Types of Tuberculosis
TB is broadly classified as active tuberculosis or latent tuberculosis. (Medical experts also recognize extrapulmonary TB, or infection that occurs outside the lungs.)
Active TB means the germs causing the infection are growing/multiplying. People who develop active TB after exposure to M. tuberculosis typically do so because their immune system is compromised by illness or medications.
“Only people with active TB can transmit the disease,” Dr. Taimur says. “When they cough, sneeze, or talk they expel invisible infectious droplets that can survive suspended in the air for some time. This means that if you live or work closely with somebody who has active TB, you are at greater risk of developing the disease.”
Most people who encounter M. tuberculosis have a strong enough immune response that they may not have any noticeable symptoms or even know they have been infected. But in these individuals, it is possible for the bacteria to lie dormant in the body.
“When you are exposed to TB, immune system cells called macrophages essentially engulf the bacteria,” Dr. Taimur explains. “Unfortunately, this isn’t always fully effective. M. tuberculosis bacteria have thick walls that protect them from being easily destroyed, and they can survive inside the macrophages for years. The immune system identifies macrophages containing these live germs and essentially walls them off inside lung nodules known as tubercles or granulomas. This is what we know as latent TB.”
Latent TB is not contagious—in fact, you may live your whole life never knowing that you were exposed to TB. However, it may reactivate in older people, as the immune response naturally wanes with age. “A depletion of immune system cells weakens the walls of the tubercles that contain TB germs and suppresses macrophage activity sufficiently that the dormant M. tuberculosis bacteria are able to proliferate,” Dr. Taimur says.
Other factors that may cause latent TB to reactivate include comorbidities like diabetes, AIDS, cancer, and rheumatoid arthritis, often because medications used to treat these conditions suppress the immune system. Chronic kidney failure, poor nutrition, and smoking also can raise the risk for TB reactivation.
Symptoms of Tuberculosis
Active TB typically causes general weakness, fatigue, unexplained weight loss, fever, and drenching night sweats. People with active TB also may experience a cough and cough up blood.
Conversely, latent TB is asymptomatic, so it is difficult to tell who may have the condition. For this reason, the U.S. Preventive Services Task Force, which provides guidance on preventive services like routine disease screening, has recommended that certain groups be tested for TB. Older adults are advised to get tested if they reside in nursing homes. Additionally, people who were born and/or resided in countries with high rates of TB at any time during their lives should be screened.
How Is Tuberculosis Diagnosed?
TB can be detected using the Mantoux tuberculin skin test or with a blood test; however, neither test can clarify whether TB is latent or active. “If your test results are positive, you’ll be referred for a chest X-ray or computed tomography to check your lungs for signs of active TB infection,” Dr. Taimur says. You also may be asked to provide a sputum sample for further testing.
Tuberculosis Complications
Without treatment, active TB causes inflammation that produces tissue damage, scarring, and cavities in the lungs. “The bacteria also can move into the bloodstream and infect virtually any organ in the body,” Dr. Taimur notes. “If TB spreads to other parts of the body, the symptoms that appear will depend on which organs are affected.”
It also is possible for people to develop drug-resistant TB, multi-drug-resistant TB (MDR-TB), or extensively drug-resistant TB (XDR-TB). The latter two are particularly serious.
Tuberculosis Treatment
Treatment strategies for TB depend on whether the infection is latent or active.
- Latent TB is treated with isoniazid or rifampin (Rifadin, Rimactane), both of which are antibiotics. “The typical treatment course for latent infection is three to six months,” Dr. Taimur says. “Be sure to carefully follow your doctor’s guidance for taking your medications, since this is the best way to prevent latent TB from progressing to active disease.” TB drugs can be toxic to the liver, so you’ll be carefully monitored for side effects and should avoid consuming alcohol, due to its potential impact on liver health. Symptoms that may indicate liver-related side effects include loss of appetite, nausea, vomiting, abdominal pain, and/or yellowing of your fingernails and the whites of your eyes. If you experience any of these symptoms while taking TB medications, immediately inform your doctor.
- Active TB may cause lung scarring and cavities if it is not effectively treated. “Successfully treating active TB takes longer compared with latent TB and requires a combination of three to four drugs due to the ability of the TB germs to develop resistance to individual drugs,” says Dr. Taimur. “In the presence of drug-resistant infection, the treatment regimen may be altered and the course might be extended.” First-line therapy usually includes isoniazid plus rifampin, pyrazinamide (Zinamide), and/or ethambutol (Myambutol). “A few weeks after starting these drugs, a person with active TB typically will start to feel better and will no longer be contagious,” says Dr. Taimur. “However, it is vital to take the medications as directed to completely eliminate the bacteria. If the drugs are stopped early, you may end up developing drug-resistant TB, which can be challenging to treat and can be passed on to others.”
Preventing Tuberculosis: What You Can Do
To help prevent TB:
- Avoid spending time in an enclosed space with anyone who has active TB until he or she has been treated for at least two weeks. At all times, follow all infection precautions put in place by medical facilities and/or nursing homes.
- Stay up to date with health advisories if you travel abroad.
- Get screened for TB if you travel abroad frequently or work in a health-care facility.
- If you are told that you have latent TB, carefully follow the directions for taking medications prescribed to treat the condition even if you do not feel unwell.
- If you are told that you have active TB, avoid close contact with other people until your doctor tells you it is safe for you to spend time with others. Do not miss any doses of your medication even if your symptoms have eased.